Fungal Foot Infections – The Ongoing Battle
Fungal foot infections are common:
Fungal foot infections are one of the most common reasons patients seek help from podiatry clinics. Conditions like tinea pedis (commonly known as athlete’s foot) are widespread, uncomfortable, and notoriously persistent. Fortunately, a range of effective treatments are available, and innovations in antifungal care continue to offer patients even better outcomes.
Understanding Tinea Pedis
Tinea pedis is a fungal infection that thrives in warm, moist environments — making feet a perfect target, especially when enclosed in shoes for long periods. Traditional treatments include topical antifungal medications such as clotrimazole, miconazole, and terbinafine. These agents are effective at clearing surface infections when used consistently and as directed.
However, a newer, promising solution has emerged: hypochlorous acid solution, marketed as Clinisept+. This innovative product shows strong antifungal properties and has been demonstrated to be effective not only against fungal infections but also against the stubborn fungal spores that often lead to reinfection.
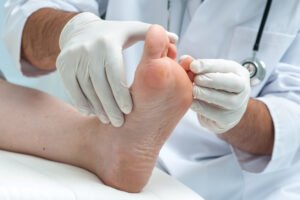
Clinisept+, a game changer for fungal foot care
One of the major challenges in managing tinea pedis is preventing reinfection. Fungal spores can linger on socks, shoes, and surfaces, even after visible symptoms have cleared.
Recent studies have shown that fabrics contaminated with T. rubrum — the most common dermatophyte causing tinea pedis — when treated with hypochlorous solution, were 99.99% free of fungal contamination. This makes Clinisept+ an incredibly useful tool for decontaminating socks, towels, and footwear, dramatically reducing the risk of reinfection.
Clinisept+ can also be used as:
-
A daily foot spray to prevent recurrent outbreaks
-
A shoe disinfectant, applied while wet to eradicate spores inside footwear
-
A general antimicrobial solution for household surfaces — safe and non-toxic for skin contact
For chronic or recurrent fungal infections, incorporating Clinisept+ into a daily hygiene routine can be an important preventative step. If you think Clinisept+ could benefit you, feel free to contact our clinic at 07 838 0003 for advice on its use.
Oral antifungal medications, how safe are they?
For more advanced or stubborn fungal infections, particularly fungal toenail infections (onychomycosis), oral antifungal medications are often prescribed. Oral terbinafine remains the gold standard, offering an impressive 80% success rate in treating fungal infections of the nail and skin. However, it’s important to be aware that studies show a 40% relapse rate within four years — another reason why ongoing preventative measures like Clinisept+ use are valuable.
Terbinafine, an allylamine antifungal agent, has been available since the early 1990s. It replaced earlier treatments like griseofulvin and ketoconazole, which were often less effective and associated with more significant side effects.
Safety profile of Terbinafine
While terbinafine has been linked to concerns over liver health, the reality is that serious liver injury is rare. It is metabolised by the liver and excreted by the kidneys. In patients with pre-existing liver disease or reduced organ function, terbinafine could present a risk of drug-induced liver injury (DILI).
Accordingly, guidelines from resources like the British National Formulary recommend:
-
Liver function tests (LFTs) before starting treatment
-
Periodic testing 4–6 weeks after beginning therapy
-
Monitoring for side effects such as nausea, vomiting, abdominal pain, or yellowing of the skin or eyes
For most patients, side effects are typically minor and include:
-
Gastrointestinal upset
-
Taste disturbances
-
Headaches
-
Mild rashes
Despite its rare risks, terbinafine is generally very well tolerated. Close monitoring ensures any potential issues are identified early, and patients are advised to report unusual symptoms promptly.
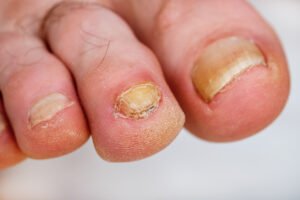
Fungal foot infections are common, but with modern treatment options — including innovative topical solutions like Clinisept+ and safe, well-monitored oral therapies — they can be managed effectively. Preventing reinfection through good hygiene practices, disinfection of clothing and footwear, and maintaining a proactive approach to foot care is crucial.
If you're struggling with persistent fungal infections or have questions about your treatment options, contact Waikato Podiatry. We are here to help you keep your feet healthy, comfortable, and fungus-free.
Suffering from a Fungal Foot Infection?
Are you are feeling like you have tried everything but are still suffering from fungal foot infection?
Do you feel like you have seen every health practitioner you can about your fungal foot infection with no results?
We have a track record of diagnosing and successfully treating cases that have previously proven difficult to resolve and we’d love to help you get the problem sorted.

